Alternative Breastfeeding Methods
Mothers who are first time moms often face challenges in getting the right latch and understanding a suitable position to feed their baby. This usually happens if the mother and baby are not give the skin to skin contact, or rooming in to initiate breastfeeding immediately after birth. As a result the baby takes time to latch and probably might have been fed the formula from the bottle. Therefore this leads to the baby refusing the breast and eventually being formula fed, and the milk supply starts reducing for the mother.
Why a Breastfed Baby May Need to Be Supplemented
Most babies can exclusively breastfeed for the first six months of life. However, there are some situations when a supplement may be necessary. Here are some of the reasons your doctor may recommend a supplement for your baby:
- Your baby is not latching on to the breast2
- Your child is not gaining weight
- Your baby has a sucking issue such as a weak suck, a cleft lip/palate, or tongue-tie
- You’re breastfeeding a premature baby3
- You’ve decided to breastfeed your adopted child
- You have a low breast milk supply
- You’re breastfeeding after breast surgery4
- You have very sore nipples
- You have stopped breastfeeding and wish to start again
- You are overcoming a c-section birth
- You are reunited with your baby after NICU
I support moms who are facing such challenges in breastfeeding and help them hop back on to exclusively breastfeeding without having to go through trauma or anxiety supporting them through their initial Motherhood days. Do you know that there are many other ways to help feed the baby if the baby is refusing the breast or even prematurely born? Unfortunately The biggest market in the mom and baby industry is the formula milks working hard to mimic the breast milk however fail in passing on the dynamic nutrition to the baby which is the enzymes, amino acids, lipids etc that help the baby’s immune system and brain development in the long run.
There are some ways a mother can successfully breastfeed her baby even without directly breastfeeding her until her supply of breastmilk increases , and this can be done by using breastfeeding substitutes that will not hinder the baby’s attachment towards the breast in the future. I have listed them below.
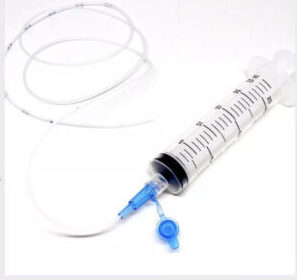
- Supplemental Nursing Systems (SNS) that uses a feeding tube either attached to a syringe or a bottle.
- Compression and Hand Expression*
- Syringe (without the needle)
- Spoon
- Cup
- Finger/ Medicine dropper
- Breast pump
How to Supplement Your Breastfed Baby
Supplemental Nursing System
A supplemental nursing system or finger feeding, can also be used with support from a specialist infant feeding advisor (for example, a lactation consultant) This is a preferred method as a breastfeeding substitute because this method helps in increasing the milk supply while the baby feeds directly at the breast but the milk comes through the tube from the container. This method also gives the mother a practice in positioning her baby correctly and improving the latch.
The supplementer consists of a container filled with your expressed breast milk, or infant formula (if medically necessary). The container connects to a tube that’s secured at the tip of your nipple. The tube acts like a straw. As your baby nurses, she draws the breast milk from your breast along with the additional milk from the supplementer into her mouth. A nursing supplementer helps to ensure that your baby gets enough nutrition6 while allowing your child to continue to stimulate your breasts to build up your breast milk supply.
Who Uses the Nursing Supplementer?
A nursing supplementer is used by mothers who are nursing adopted babies, as well as by mothers who are relactating (reestablishing a milk supply after a premature weaning). Nursing supplementers are also used with preemies or babies with various kinds of sucking problems that prevent them from getting enough milk directly from the breast. To use a supplementer, the baby must be willing and able to latch onto the breast.
Different Types of Nursing Supplementers
Talk to a lactation consultant or counselor before using a nursing supplementer. She can help you decide if this is the best choice in your situation. She will also help you resolve the breastfeeding problem that has created the need for a supplementer.
Hand expression
If you have a newborn who is not feeding well initially ,hand express your colostrum 8 to 12 times every 24 hours (including at night) to help stimulate your breasts to make milk. The sooner you do this and the more often you do this after your baby’s birth, the more milk you will make. Any colostrum you collect can be given directly to your baby via a syringe or a
spoon. Giving your baby colostrum will also encourage them to feed from your breast.
How to hand express your breast milk
- To collect your expressed breast milk, you will need a clean, sterilized container,preferably glass container. If you are expressing colostrum/milk, you will also need a clean, sterilized syringe. Make sure you have these items ready before you start.
- Make yourself comfortable and try to relax. Warmth will help, so try expressing yourself in the shower or bath first. You can gently massage your breasts with a warm flannel.
- Use your hand to cup one of your breasts. Your hand should be in a ‘C’ shape around the nipple, with four fingers under your breast and your thumb at the top. Your thumb and fingers should be about 2 to 3cm away from the areola (the darkened area of skin around
your nipple).
- Use your thumb and index finger to gently squeeze. Release the pressure and then repeat to create a rhythm. This shouldn’t hurt. Avoid sliding your fingers over your skin as this may cause discomfort. If the colostrum/milk doesn’t flow, try moving your fingers slightly
towards the nipple or further away, finding the spot that works best for you. You could also try gently massaging your breast.
- Collect your colostrum/milk with the sterilized syringe, and if necessary, decant to the larger sterilized container. Colostrum is very concentrated and will come out of your breast drop by drop. At first, only a few drops will come out at each session which is enough for the new born, with practice and time, the volume will increase. When the drops slow down, move your fingers round to try a different sections of your breast and repeat.
- Repeat the process for your second breast.The amount of colostrum you collect when you express can vary from just a few drops to a teaspoonful. As your colostrum increases in volume and starts to change to mature milk, you may wish to use a breast pump or supplemental nursing system.
Syringe feeding
Syringe feeding can be used when you need to give your baby small amounts of colostrum or expressed breast milk (less than 5ml at a time). This is usually during the first couple of days after your baby’s birth.
How to syringe feed your baby
- Use a small, sterile syringe and place no more than 0.2ml into your baby’s mouth at a time. Feed the milk in between their gum and cheek or onto their tongue.
- Allow your baby to swallow the milk before giving them another 0.2ml and continue to do this until the feed has
ended.
- Do not allow your baby to suck on the syringe and do not squirt the milk into their mouth.
Infant feeding syringes have free-fastening lid which must be removed
before giving expressed colostrum or milk to your baby.
- Always keep syringes and lids away from babies and children.
Spoon feeding
You may wish to sterilize and use a small, steel spoon rather than a syringe when feeding small amounts of colostrum to your baby. You can express your milk directly onto the spoon and then offer it straight to your baby.
How to spoon feed your baby
- Gently offer the spoon to your baby’s lips and wait.
- Your baby will then sniff the milk, push their tongue forward and start to lap or drink the milk. Do not pour the milk into your baby’s mouth.
Cup feeding
Babies can drink from a cup, even small babies. Cup feeding encourages your baby to use their tongue and lower jaw in a similar way as they would when breastfeeding. It also gives your baby more control over how much they drink and how quickly they drink. Babies are also able to smell and enjoy the milk when using a cup. Any
feeding cup can be used if you are offering your baby more than 5ml of milk during a feed.
How to cup feed your baby
- If you are at home, sterilize a small feeding cup. The cup should never be more than two thirds full with milk.
- Direct the lip of the cup towards your baby’s upper lip and gums, with it gently touching or resting on their lower lip
(make sure you don’t apply any pressure to their lower lip). This will gently stimulate your baby’s natural rooting reflex.
- Slowly tip the cup so that the milk touches your baby’s lip and then wait. Your baby will then sniff the milk, push their tongue forward and start to lap or drink the milk. Gently tip the cup as your baby drinks, so that the milk is always just on the rim of the cup.
- Leave the cup in the correct position during the feed. Do not remove the cup when your baby has occasional pauses. Allow your baby to resume feeding when they are ready and let them set their own pace (follow your baby’s cues).
- Continue to offer the cup until your baby shows you that they have had enough milk.If you decide to cup feed your baby, you may need to give them smaller but more regular feeds to make sure they have enough to drink
General Guidelines for Cup Feeding Your Baby
Sit the baby upright on your lap with the baby’s head supported, at a 45 degree angle or taller. Baby should not be flat on its back.
Use a small medicine cup or shot glass.
Place the edge of the cup gently on the baby’s lower lip.
Bring the liquid to the baby’s lower lip so the baby will lap it up like a cat drinking milk from a bowl. Do not pour the liquid in baby’s mouth
It is important to maintain the level of the liquid as best as possible so the baby can continually lap it up.
Go slowly as the two of you learn how to do this. Eventually, this can become a very fast and efficient way of feeding until the baby learns to take the breast, and this is a good method to use to avoid artificial nipples and teats. This method also encourages tongue extension which is helpful training for babies who have had tongue tie revision or therapy for shallow latching.
Infants who are given supplements in a cup are less likely to get nipple confused and more likely to go on to successfully breastfeed. Research has shown that not only is it possible for preemies to drink from a cup, but they also maintain a more stable blood-oxygen-level during cup-feeding than during bottle-feeding.
General Guidelines for Syringe Feeding Your Baby
Spoon, Dropper, or Syringe Feeding: Milk placed on a spoon, in a dropper, or in a syringe can be slowly placed into the baby’s mouth in very small amounts.10 Each time the baby swallows, a little more is introduced into the mouth until the feeding is complete. These types of feedings are best for very young infants who only require a small amount of supplementation.
Fill the syringe with expressed breast milk.
Sit the baby upright on your lap with the baby’s head supported, at a 45 degree angle or taller. Baby should not be flat on its back. Stroke baby’s face to stimulate gape response. Gently drag your finger down from the tip of the baby’s nose to the chin. When the baby opens wide, offer a finger to suck, pad side up.
Once the baby begins to suck, introduce a syringe to the corner of the mouth. Point the tip of the syringe into the cheek. The tip is rigid. Do not allow the tip of the syringe to touch the gums.
Responsively depress plunger as baby is sucking on finger. The baby is only able to swallow small amounts. The baby needs time between pulses of milk to coordinate breathing. One pulse of milk should be followed by a swallow and two or three sucks.
Cup feeding for supplementation off the breast may be a good choice for several reasons. Cups are easy to sterilize unlike rubber nipples. Cup technology is available around the world in all cultures. Cup feeding teaches baby oral skills that he will use for a lifetime. Babies who are cup feeding learn tongue extension, which is a useful skill for drawing the breast deep into the mouth to nurse.
You can also use a feeding syringe to supplement a baby at the breast. Insert the tip of the syringe into baby’s mouth while he is latched on, and depress the plunger to reward the baby when he sucks.
Finger Feeding: If your baby is having trouble latching on the breast, or if you have extremely sore nipples that need a break from breastfeeding, you can try finger feeding.7 Finger feeding is similar to breastfeeding with a nursing supplementer device. Except, instead of attaching the supplementer to your nipple, you attach the tube to the tip of your finger. Then, you place your finger in the baby’s mouth. As your child sucks on your finger, the feeding will be drawn from the supplementer into her mouth.
Bottle-Feeding: Bottle feeding is perhaps the most common way to provide a supplement provided that paced bottle feeding is adopted. A bottle with a slower flow nipple is usually better for a breastfed baby.Faster flow nipples make it easier to get milk out of the bottle, which for some babies can lead to a preference for the bottle. If you’re having trouble deciding on a bottle, talk to a lactation counselor for recommendations
Which Alternative Feeding Method Is The Best?
A nursing supplementer is the preferred method for supplementing a breastfed baby if the child can latch on and nurse. Finger feeding is a good alternative to a nursing supplementer when breastfeeding is not possible. Bottle feeding may be the easiest way to supplement a baby, but it’s the method most likely to undermine breastfeeding.5 Some infants may develop nipple confusion or refuse to breastfeed once a bottle is introduced.
Which Breastfeeding Alternative Method to Choose
When to give supplements with a cup (or a spoon or eyedropper):
- Baby has not yet learned how to latch onto the breast
- Baby is having problems with nipple confusion
- It’s likely that baby will need supplementation for a relatively short period of time
- When an older breastfed baby refuses the bottle
When to use a supplementer:
- Baby is able to latch onto the breast but can’t get sufficient nourishment from breastfeeding alone.
- When training a baby to suck correctly at the breast (get help from a lactation consultant).
- The need for supplements is likely to continue for several weeks. (It may take a few days to become comfortable with using a supplementer, which is why many advisors suggest cup-feeding when the need for supplements is only short-term.)
- When you wish to supplement baby at the breast and avoid the time and effort required to give baby additional feeding after nursing sessions.
- Relactating or nursing an adopted baby.
When to use finger-feeding:
- Baby has not yet learned how to latch onto the breast
- When teaching a baby to suck correctly (get help from a lactation consultant)
A lactation consultant can help you decide which bottle alternative method will work best for you and your baby and can help you locate and purchase special feeding equipment. She will also help create a plan for gradually eliminating the need for supplements.
Breast Pump
This alternative feeding methods commonly used to increase milk supply and substitute with expressed milk or formula (in specials cases) . Although this method is beneficial in increasing the milk supply , the method of using a breast pump is not suitable for all. It is the most common choice of a working mother wishing to return back to work. Choosing a breast pump involves a good research and advice from the lactation consultant . There are different types of breast pumps, sizes of the flanges should be chosen carefully to keep up the efficiency for pumping milk. There are numerous resources available some of which I have listed below however will not be covering this in detail in this section.
Complete Beginner’s Guide to Using a Breast Pump – Exclusive Pumping
How to Tell if Your Breast Pump Flanges Fit (verywellfamily.com)
How Do I Know What Size Flange to Use with My Breast Pump? – Milky Mama (milky-mama.com)
A Warning About Alternative Feeding Methods
Cup, spoon, syringe, and dropper feedings must be carried out carefully. These methods are not as safe as using a nursing supplementer or a bottle. If too much milk is given to the baby at one time, or the supplement is allowed to flow continuously into the baby’s mouth, it could go into the child’s lungs. The inhalation, or aspiration, of a supplement into the lungs is a very dangerous situation.13 If your doctor or lactation consultant recommends cup, spoon, syringe, or dropper feedings, be sure that you are taught the correct technique for these feedings, and that you feel comfortable using them.
Additional options for older babies (4+ months)
After 4-6 months, there is really no need to introduce a bottle — babies this age can generally handle a cup just fine (expect to help out in the beginning, though). If you need to, try different types of cups to see what works best for you and baby: regular cup (try different sizes), no-spill cup, cup with straw (or a cup with a built-in straw), and sports bottle are all options that different babies use.
Syringe sizes 1ml to 50ml available
Infant feeding tube 5fg, 6fg, 8fg
Cup – shot glass size upto 50ml & 900ml
Resources & Information
https://www.verywellfamily.com/alternative-feeding-methods-431905
- Cup Feeding from the Breastfeeding Committee for Saskatchewan
- Cup Feeding Instructions and FAQs from foleycup.com
- Comparison of the Safety of Cup and Bottle Feedings in Premature Infants Whose Mothers Intend to Breastfeed information on study by Kathleen A. Marinelli, MD, IBCLC; Georgine S. Burke, Ph.D; Virginia L. Dodd, MS, RNC. The full article can be found here.
- Feeding by cup, paladai or spoon (see p. 206 of PDF file – note that this file is very large and will likely take a long time to load if you have a slow connection) from the WHO document Managing Newborn Problems: a guide for doctors, nurses and midwives.
- Physiologic Stability of Newborns During Cup- and Bottle-feeding by Cynthia R. Howard, et al., from Pediatrics, Vol. 104 No. 5 Supplement, November 1999, pp. 1204-1207.
- SoftFeeder (with link to Instructions) from Medela
Finger feeding
- Finger and Cup Feeding by Jack Newman, MD, FRCPC
- Finger-Feeding with a Feeding Tube from the Breastfeeding Committee for Saskatchewan
- Finger-Feeding with an Oral Syringe from the Breastfeeding Committee for Saskatchewan
Weaning back to the breast from other feeding methods
Transitioning baby from formula feeding to breastfeeding @
includes links to information on reducing supplements and transitioning to the breast from bottles, nursing supplementers, Haberman feeders, etc.
https://kellymom.com/ages/newborn/newborn-concerns/alternative-feeding/